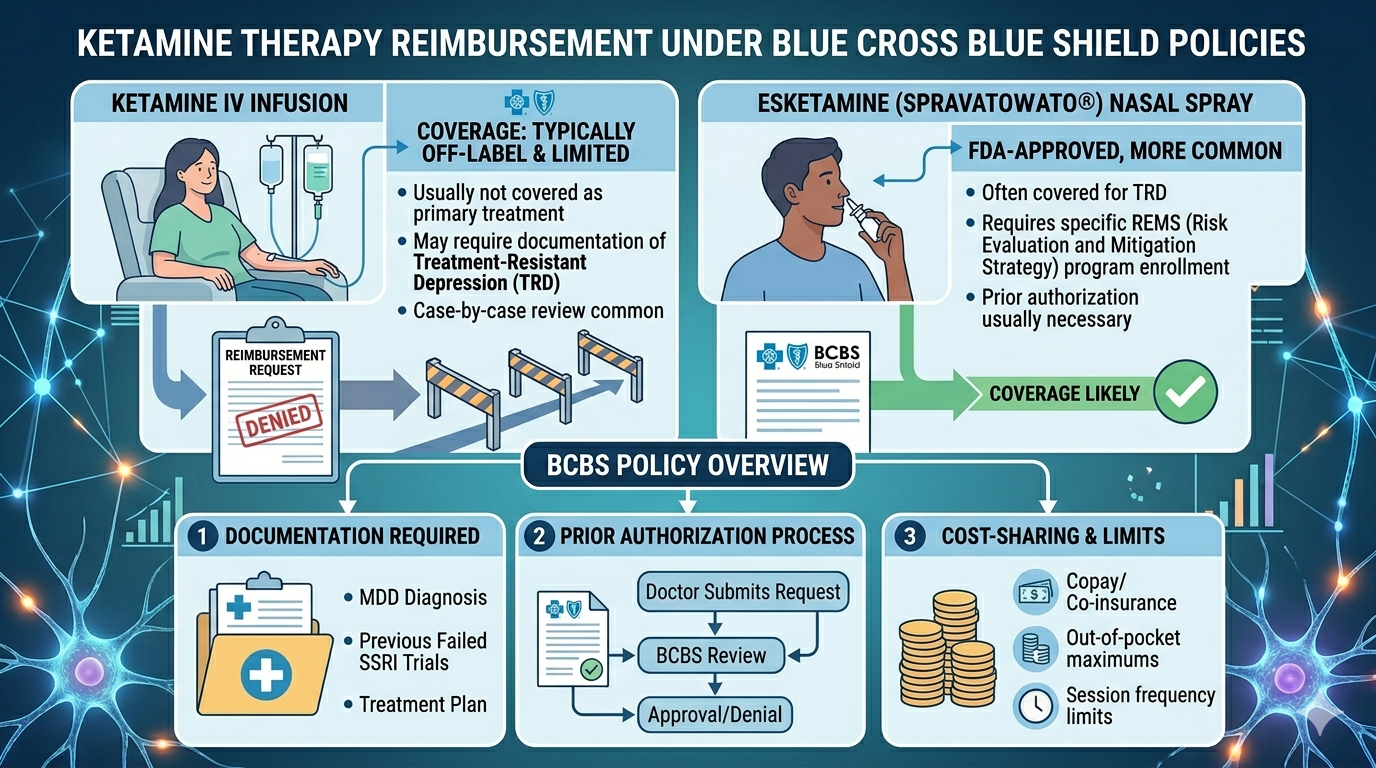
Ketamine Therapy Reimbursement Under Blue Cross Blue Shield Policies
Does Blue Cross Blue Shield cover ketamine treatment is a common question for patients exploring advanced options for depression and related mental health conditions. As ketamine therapy becomes more visible in psychiatric care, questions around insurance reimbursement, eligibility, and out-of-pocket costs have become more important. Unlike traditional medications, ketamine treatment involves different administration methods and clinical protocols, which can affect how insurers evaluate coverage. Understanding how reimbursement works under Blue Cross Blue Shield policies helps patients make informed decisions about access, affordability, and treatment planning.
How Insurance Coverage Applies to Ketamine Therapy
Insurance coverage for ketamine therapy does not follow a single standardized model. Instead, reimbursement depends on how the treatment is classified within a plan. Some components of care may be considered medically necessary, while others may fall outside typical coverage categories.
Health plans often distinguish between FDA-approved treatments and off-label therapies. This distinction plays a key role in determining whether services are eligible for reimbursement. Coverage decisions are also influenced by diagnosis, provider credentials, and documentation of prior treatment attempts.
Blue Cross Blue Shield Policy Structure and Variability
Blue Cross Blue Shield operates through a network of regional providers, each managing its own plans and policy details. This structure means that coverage for ketamine therapy can vary depending on the specific state plan and individual policy terms.
Some plans may offer partial reimbursement for certain aspects of treatment, while others may not include ketamine therapy within their covered services. Reviewing the summary of benefits and speaking directly with the insurer is often necessary to understand what is included under a specific plan.
Medical Necessity and Eligibility Criteria
For any treatment to be considered for reimbursement, it must typically meet criteria related to medical necessity. This involves demonstrating that the therapy is appropriate for the patient’s condition and that other standard treatments have been tried without sufficient success.
In the context of ketamine therapy, documentation often includes a history of treatment-resistant depression or similar diagnoses. Providers may need to submit clinical records, prior medication history, and treatment plans to support authorization requests.
Prior Authorization and Approval Process
Many insurance plans require prior authorization before approving coverage for specialized treatments. This process involves submitting detailed clinical information for review before therapy begins.
The approval process may take time and does not always result in full coverage. Patients and providers often work together to prepare documentation that aligns with the insurer’s requirements. Even when authorization is granted, it may apply only to specific components of care rather than the entire treatment program.
What Portions of Ketamine Treatment May Be Covered
Coverage for ketamine therapy is often divided into separate components rather than treated as a single service. This can include evaluation visits, monitoring, and certain clinical procedures associated with treatment sessions.
In some cases, office visits or mental health consultations may be eligible for reimbursement, while the ketamine administration itself may not be covered. This distinction can affect the overall cost structure and should be clarified before beginning treatment.
Out-of-Pocket Costs and Financial Planning
When insurance coverage is limited or partial, patients may be responsible for a significant portion of the treatment cost. Understanding the breakdown of expenses helps in planning and avoiding unexpected financial strain.
Costs can vary depending on the number of sessions, type of administration, and provider setting. Some clinics offer payment plans or financing options, but these are separate from insurance reimbursement and should be reviewed carefully.
Importance of Verifying Coverage Before Treatment
Verifying insurance coverage in advance is a critical step before starting ketamine therapy. This includes confirming benefits, understanding authorization requirements, and identifying which services are eligible for reimbursement.
Patients are encouraged to contact their insurance provider directly and request detailed information about mental health benefits and coverage limitations. Clear communication between the patient, provider, and insurer can help reduce confusion and support better decision-making.
Evolving Landscape of Insurance and Ketamine Therapy
Insurance coverage for ketamine therapy continues to evolve as research expands and clinical use becomes more established. Policies may change over time, reflecting new evidence, regulatory developments, and shifts in treatment guidelines.
While coverage remains variable, there is growing attention on how newer therapies fit within existing insurance frameworks. Staying informed about policy updates can help patients and providers navigate this changing landscape more effectively.
Conclusion
Questions around whether Blue Cross Blue Shield covers ketamine treatment reflect broader challenges in aligning innovative therapies with traditional insurance models. Coverage depends on multiple factors, including plan details, medical necessity, and the structure of the treatment itself. While some aspects of care may be eligible for reimbursement, others may require out-of-pocket payment. Careful review of policy terms and proactive communication with providers and insurers can help patients better understand their options. As mental health treatment continues to advance, insurance frameworks are gradually adapting, but variability remains an important consideration.




Leave a Reply